
The Boredom Breakthrough: Why “Rest” Isn’t Enough for Healing



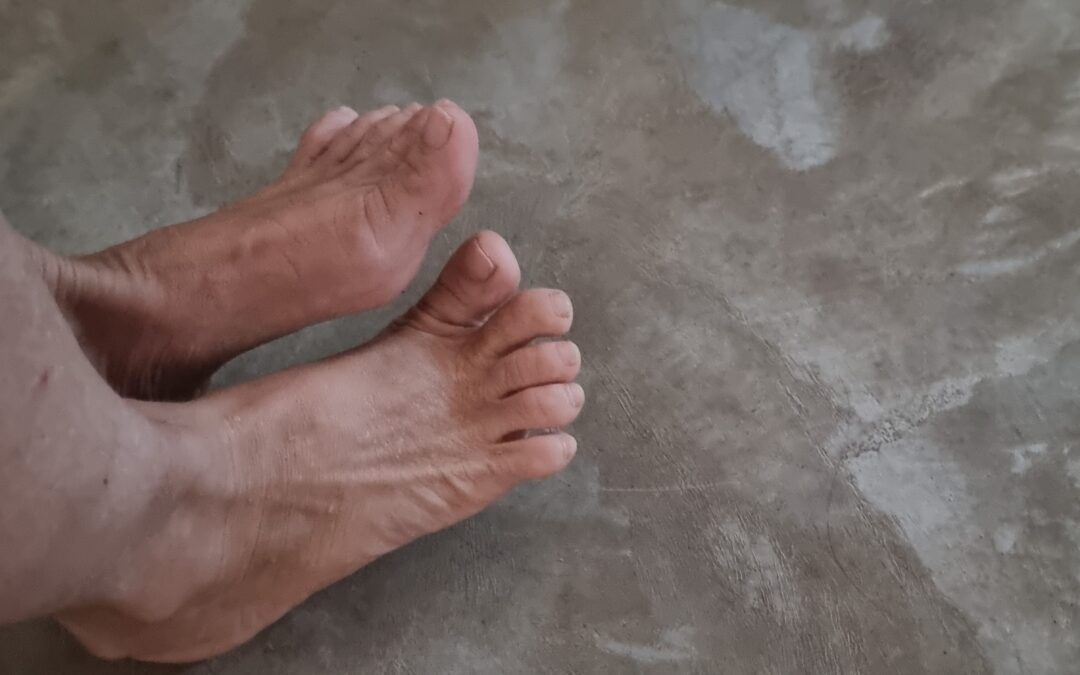




I didn’t leave Nepal on the trekking boots I arrived in. I left in a wheelchair, with a pair of crutches balanced across my lap and a right foot that felt like a heavy, silent stranger.
By this stage, I had already received my MRI results. In my professional life, I’ve reviewed thousands of these reports, but reading your own is a surreal experience. The words “global disc bulge” and “foraminal stenosis” jumped off the page. It wasn’t just one level; both L4/L5 and L5/S1 were involved, creating a mechanical bottleneck for the nerves traveling down my leg.
This explained the “foot drop”—a term that sounds far more clinical than it feels when you’re trying to navigate an airport and your toes simply refuse to lift.
Being an expert in your own injury is a double-edged sword. Having the report meant I couldn’t hide behind “maybe it’s just a strain.” I knew the structural reality of the stenosis and the multi-level involvement.
As a pain practitioner and physiotherapist, I have spent decades treating this exact pathology. But sitting in that terminal, the “Expert” was nowhere to be found. I was just a woman whose body had reached its absolute threshold. My “Expert Brain” became a relentless noise machine, searching internal archives for surgical outcomes and long-term prognosis.
My Physio Brain shouted: “You’ve seen the report. There is significant foraminal narrowing. You need a surgical consult immediately. You are being reckless.”
My Patient Body whispered: “I need warmth. I need the ocean. I need to feel safe before I can heal.”
In Acceptance and Commitment Therapy (ACT), we talk about “Psychological Flexibility”—the ability to stay in contact with the present moment and choose actions based on our values, even when difficult emotions or sensations are present.
I had a choice. I could fly back to South Africa and head straight for a neurosurgeon—a path that a multi-level stenosis report certainly justified. Or, I could follow through with my sabbatical plans and fly to Sri Lanka.
To many, flying to a tropical island with a foot drop and confirmed spinal stenosis looks like denial. To me, it was a calculated clinical risk. I knew that my nervous system was in a state of high-alert (the “Freeze” response). I knew that while the MRI showed structural narrowing, the experience of pain is heavily influenced by the state of the nervous system. I wanted to see if, by resourcing my body with the safety of the ocean, I could settle the neural inflammation enough to regain motor function & reduce this constant, unremitting and excruciating nerve pain.
I’ve spent my career telling patients: “You are not your MRI. Your body is a self-healing organism. Trust the biology.”
Now, it was time to see if I actually believed it.
I chose the flight to Colombo. I chose the uncertainty of the “Path of Trust” over the perceived safety of the “Path of Control.” I chose to believe that if I could lower the “threat” level in my brain, my body would have the energy it needed to manage the inflammation at those levels and begin the slow work of neural repair.
I boarded that plane not knowing if I would ever walk properly again, but knowing that for the first time in my life, I was truly walking my own talk.
What’s Next?
The flight was grueling, and the arrival in Weligama was a crash course in humility. In my next post, I’ll share what happened when I finally touched the Indian Ocean—and why “The Blue Pharmacy” became my most important clinical discovery yet.
Tracy’s Clinical Note: If you are navigating a similar injury, please remember that this is my personal journey. While I chose to proceed with my plans despite the MRI findings of multi-level stenosis, I remained hyper-vigilant for “Red Flags” like Cauda Equina Syndrome. Trusting your body also means knowing when it truly needs expert medical intervention.
Contact: Tracy Prowse at tracyprowsephysio.co.za
Registration Number: PH55586
(+27) 083 408 8582
tracy@prowse.org
Mondays - Fridays: Online Consultations
Mondays, Wednesdays, Fridays: The Gatehouse, 91 Brommersvlei Rd, Constantia, Cape Town, 7806
Saturdays: 6 Krige Street, Stellenbosch, 7600
Mon., Wed. & Fri.: 9:00 - 18:00 (Constantia)
Sat.: 9:00 - 17:00 (Stellenbosch)
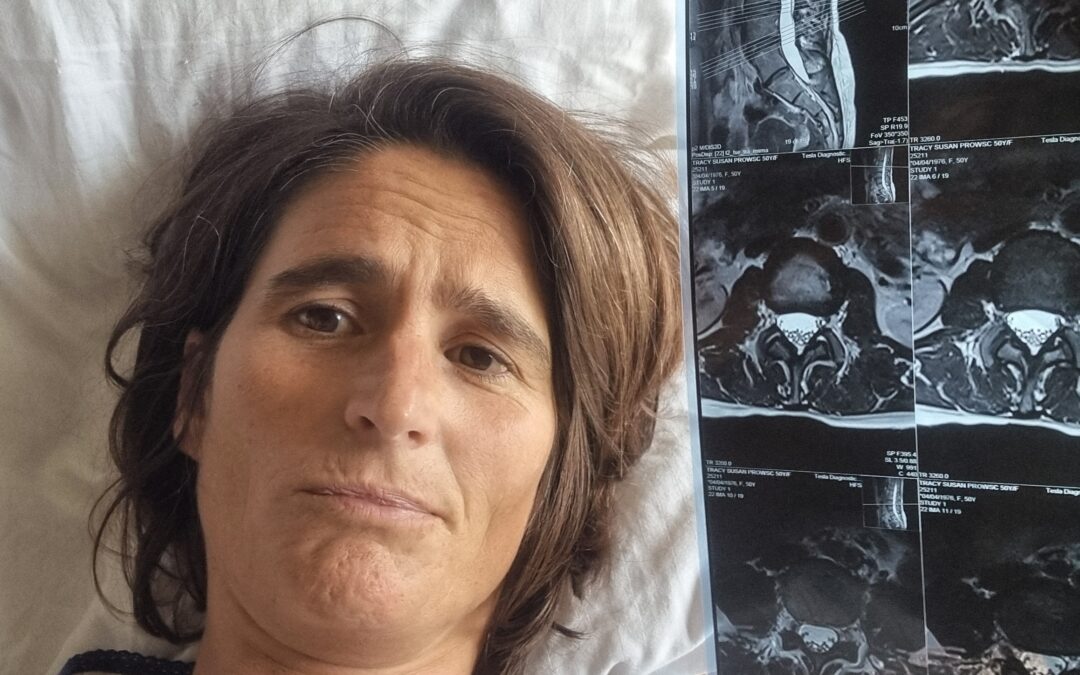
In my last post, I wrote about the “mountain within”—the bracing patterns and the “Freeze” response I navigated while trekking the Annapurna Circuit. I spoke of the lessons learned at 5,400 meters about pain being a language of survival.
Today, I am writing from a hospital bed in Kathmandu. The “residual sciatica” I mentioned didn’t settle. It roared. I am currently navigating a full-blown L5/S1 nerve root compression, a foot drop, and pain so unremitting it required IV pethidine to break the cycle. My MRI shows a global disc bulge and foraminal stenosis. As a physiotherapist and SE practitioner, I’ve spent years telling patients: “You are not your scan.” Now, I am the one tasked with living that truth.
In ACT (Acceptance and Commitment Therapy), we talk about context. My disc didn’t just “give out” because of a bouncy jeep ride. It reached its threshold after a perfect storm of “Danger-In-Me” (DIM) cues:
The Biological Drain: I started the trek recovering from Norovirus, then took Diamox (a diuretic), which likely contributed to disc desiccation.
The Emotional Load: At my physical limit, I received news that my father was unwell. My system, already taxed, immediately manifested this as nausea and diarrhea—the gut-brain axis screaming for a halt.
The Final Push: After the harrowing descent, I “ran” that last day down the mountain without my trekking poles. That burst of “High Sympathetic” energy felt like triumph, but it was likely the last bit of fuel my adrenals had to give.
By the time I hit the bouncy jeep to Pokhara, my body had no more “give.” The bracing that protected me on the mountain became the very thing that compressed the nerve.
Right now, my body is a fortress. The inflammation is a biological “splint,” and the pain is a high-decibel alarm. My medical team is providing the “top-down” support—corticosteroids, NSAIDs, and muscle relaxants. This is the medical window —a pharmacological hand-hold that allows my nervous system a moment of quiet so I can begin the “bottom-up” work.
The question I’m holding is: How do I signal safety to a body that feels betrayed?
1. Somatic Tracking and the “Thaw”
Last night, I practised a somatic review of the trek. I revisited the triggers—the stairs, the news about my dad, the fear of the insurance company. I allowed the tears to come. In Somatic Experiencing, we know that suppressed emotion is simply stored “incomplete” energy. By crying, I am allowing the “Freeze” to thaw, letting the sympathetic charge move through me rather than staying locked in my spine.
2. Finding Quiescence
My SE training taught me about Quiescence —a state of purposeful rest that is deeper than just “not moving.” It is an active surrender. I am currently in a state of forced stillness. I can fight it, or I can use it as a sanctuary. I am choosing to see this hospital bed as a “Resourcing” station.
3. ACT: Acceptance vs. Resignation
Acceptance doesn’t mean I like the foot drop. It means I stop wasting energy fighting the fact of it.
* The Values: My value is resilience and body-wisdom.
* The Action: Sometimes, the most “courageous” action isn’t climbing a mountain; it’s being willing to lie still, breathe into the discomfort, and trust the phagocytes to do their work
It’s easy to spiral into “Why did I push?” and “I should have turned back.” I’ve even projected that blame onto my husband (and promptly apologized—blame is just pain looking for a home).
But the reality is: This is the path now. Being in a hospital in a foreign country is a massive “Danger” cue. To counter it, I am looking for “Safety” cues:
* The relief of the insurance being sorted after a hard fight.
* The warmth of my husband’s hand.
* The fact that I discovered actually have severe cervical stenosis and multi level disc bulges in my cervical spine —which looks worse on paper—isn’t causing me any trouble at all, and never has! This proves to me (not just because the research tells me this but because this is my lived experience) that physiology is fluid, not fixed.
My body spent weeks trying to keep me alive on a mountain. It did a spectacular job. Now, I am talking to my cells. I am telling my lower back: “We are off the mountain. We are at a lower altitude. We are cared for. It is safe to stand down.”
Recovery isn’t just the absence of a bulge; it’s the return of a sense of internal safety. Whether I end up in surgery or manage this conservatively, the goal remains the same: to move from a state of survival back into a state of being.
For now, there is only the breath, the bed, and the slow, miraculous process of healing.
Contact: Tracy Prowse at tracyprowsephysio.co.za
Registration Number: PH55586
(+27) 083 408 8582
tracy@prowse.org
Mondays - Fridays: Online Consultations
Mondays, Wednesdays, Fridays: The Gatehouse, 91 Brommersvlei Rd, Constantia, Cape Town, 7806
Saturdays: 6 Krige Street, Stellenbosch, 7600
Mon., Wed. & Fri.: 9:00 - 18:00 (Constantia)
Sat.: 9:00 - 17:00 (Stellenbosch)